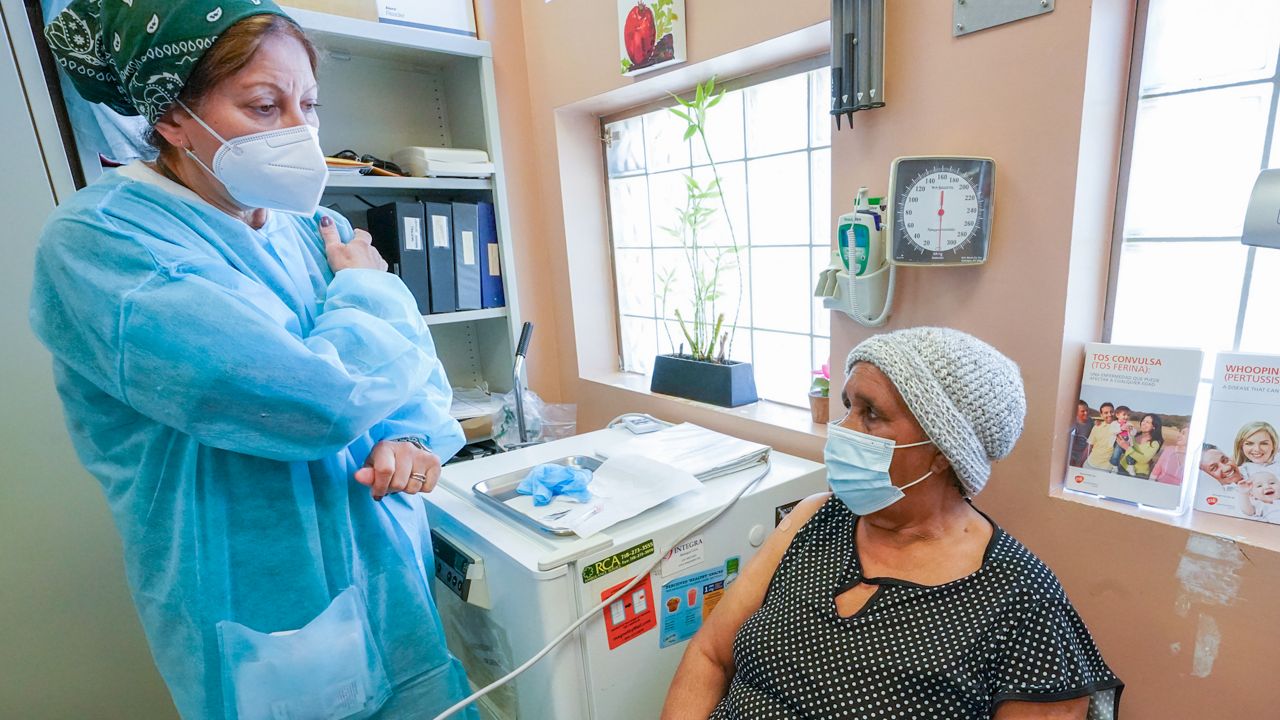
Community health centers are crucial to the Biden Administration’s efforts aimed at making sure anyone, anywhere, can get the COVID-19 vaccine.
The White House is hoping these community centers will reach many of the hesitant and vaccine resistant in order to reach President Joe Biden’s latest goal – 70% of U.S. adults vaccinated with at least one shot by July 4th.
With the help of these community health centers, White House officials say a majority of first doses are now going to people of color.
But health care workers in these centers say the demands placed on them throughout the pandemic and now during vaccine distribution efforts, continue to expose a persistent weakness: They need more help.
“Since March of last year, I don't know how much we have slept,” Dr. Miriam Vega, CEO of the Joseph P. Addabbo Family Health Centers in Brooklyn and Queens, told Spectrum News.
The Addabbo clinics are part of a network of Federally Qualified Health Centers, meaning they rely on federal funding through the Health Resources & Services Administration to provide health care to under-resourced areas and people. The clinics had to rapidly pivot to telehealth at the start of the pandemic, which eventually led to the furloughing of 100 members of their staff.
“We went from being paid $180 for face to face visits, to being paid $9.16 for a telemedicine visit," Dr. Vega said. "So financially, we took an enormous hit."
As the federal government changed billing to accommodate the pandemic, and the need for more testing sites increased, Vega said they were able to rehire some staff. Then as the vaccine distribution ramped up, they needed even more help.
“You have a staff of pretty much 10 people doing the work of 30. It was pretty challenging,” said Marie Gallant, a registered nurse and the associate director of nursing for the Joseph P. Addabbo Family Health Centers. “One doctor used to have two staff members assigned to them, now sometimes you have one staff member assigned to two doctors.”
It’s a similar story nationwide: At the South Central Family Health Centers’ 9 clinics serving the Los Angeles area, they haven’t been able to hire new staff fast enough.
“There's about a 25,000 primary care provider shortage in California alone," Dr. Jose Luis Perez, chief medical officer for South Central Family Health Centers, said. "So when this pandemic started, we were already behind the curve,”
“We have about 40 positions that are available that we haven't been able to fill in the last six months," Dr. Perez said, noting that includes medical assistant, provider and nurse positions.
Large, well-funded, hospital systems also need more providers and nurses, which makes the problem even more acute in these cash-strapped health centers.
“We don't get the same amount of doctors wanting to come and practice," Dr. Perez said. "At some point, even if you have a social conscience and you want to do the best as a young doctor or your young nurse practitioner, your family comes first, having a good salary to support your needs personally."
"Workforce has been an issue that we've been dealing with for as long as I have been a medical officer over the last twenty years," Dr. Perez added. "The pandemic only served to expose that major weakness in the structure of the system.”
According to the National Association of Community Health Centers, many centers across the country have adapted to the increased demands brought on by the pandemic and the vaccine distribution, but staffing continues to be a growing challenge. A recent survey done by the organization found that 48% of health centers need more staff, compared to 35% at the beginning stages of the vaccine rollout. The report points to health care worker burnout, after more than a year of responding to the pandemic.
“We're, at the moment, multitasking at a higher level than we had seen before. So our brains are working overtime,” said Vega. Not to mention coping with their own coronavirus related losses and illnesses.
Federal funds from the American Rescue Plan are helping to keep these centers afloat. Both Vega and Perez said they were also able to get some help from nursing students through partnerships with nearby colleges. But more creative, out-of-the-box solutions may be needed to sustain community health centers into the future.
Perez said programs like the National Health Services Corps should be drastically expanded and pointed to medical school requirements in his home country of Nicaragua. “In Central America where I'm from, medical doctors, the year before they graduate, they get sent into very poor communities,” he said. “The idea is, you do your practice, maybe you'll fall in love with the people that you take care of and you end up spending your professional career there.”
Gallant said she hopes more pipeline programming is created for high school students. Nursing didn’t become her passion until recently. Gallant’s children are now grown, so she said her focus is on helping her community thrive. So for now she and others like her will continue to show up.
“There was a job that needed to be done here and my community needed it,” said Gallant. “So you cannot just jump ship. Who's going to do it?”